Essential Movement Qualities: Hip Internal Rotation
By: Phil Loomis
Hip internal rotation (HIR) is very important in sport and performance training. Here are a few examples:
- During a change of direction or when making a cut HIR helps decelerate the body while also loading the hip allowing for a powerful reacceleration.
- When sprinting HIR allows an athlete to maximally extend their hip and get over the stance leg at terminal stance/toe off, thus improving stride length.
- For rotational athletes in golf, baseball, tennis, etc. HIR is crucial for optimizing force transfer from the lower extremity to the upper extremity.
- When squatting adequate HIR allows the femoral hide to remain centrated within the acetabulum allowing for a “cleaner” pattern free of compensation at the lumbar spine/knees/ankles.
So, all that said, hip internal rotation is an extremely important element of efficient athletic movement, but…
Anecdotally, HIR is often limited in many male athletes. And in some cases (hockey) it’s nearly non-existent.
Why do we need IR? Or more accurately what happens when an athlete doesn’t have adequate hip internal rotation?
The hip needs full IR for proprioception. We must have full mobility so that the mechanoreceptors can see the entire picture (rather than a distorted view) and provide an accurate response (motor control) for what is needed in the correct proportion and at the right time.
Limitations in hip total rotational range of motion (IR+ER) have been linked to increased risk for adductor strain in professional soccer players and limitations in HIR has been associated with increased lower back pain in professional tennis players.
Decreased hip internal rotation increases the risk of back and abdominal muscle injuries in pro baseball players.
Xinning et al., found decreased hip internal rotation and total arc of motion are associated with in-season hip, hamstring, and groin injuries among MLB players. Additionally, this research team concluded, “players with decreased internal rotation of the hip may be plagued with lower throwing velocity as the transfer of energy between the lower and upper extremity in the kinetic chain is altered.”
In our modern youth sport culture, young athletes are exposed to repetitive motions from a single sport nearly year-round. When an athlete doesn’t have the requisite hip internal rotation to accommodate the demands of their sport (HIR force greater than available HIR) it will likely result in osseous (bony) changes and damage to soft tissue structures such as the labrum of the hip.
In the aforementioned research linking limitations in HIR to low back pain in tennis players Vad et al., concluded: “due to the repetitive pivoting at the lead hip, the cycle of microtrauma and scar formation leads to capsular contracture and subsequent reduction in internal range of motion”.
In 2013 Philippon et al., imaged the hips of 61 youth hockey players from 10-18 years old, and found that:
In Peewees (10-12 y/o), 37% had Femoral Acetabular Impingement and 48% had labral tears
In Bantams (13-15 y/o), 63% had FAI and 63% had labral tears
In Midgets (16-19 y/o), 93% had FAI and 93% had labral tears
The researchers concluded: “Properties inherent to ice hockey likely enhance the development of a bony overgrowth on the femoral neck, leading to cam FAI.”
Reagan et al., measured humeral retroversion in 294 kids between the ages of 8-16 and concluded: “The loss of internal rotation and gains in external rotation may be more strongly related to adaptive changes in proximal humeral anatomy than to changes in the soft tissues. Children showed baseball specific adaptations at a very young age.”
Putting all of this commentary and research together it seems fair to say that the functional demands of a sport likely contribute to soft tissue restrictions initially. And when these adaptations aren’t countered via a mobility/motor control process in addition to an authentic off-season, the IR force exceeds the usable HIR leading to bony adaptations that close down efficient joint motion and “chew-up” soft tissue structures like the labrum of the hip in the process.
While my topic is centrally focused on hip internal rotation, I threw in the Reagan et al. research pertaining to the shoulder because it elicits a very important point to touch upon…
We should never assume side to side differences in joint motion or the lack of “normative” range at a specific joint will lead to injury. In fact, the opposite may actually be true as some of these structural adaptations may deliver protective qualities. And in the case of baseball pitchers, the ability to get into the “layback” position is essential to throw hard. So, these structural adaptations may offer performance enhancing benefits as well.
That said, if asymmetries or reduced joint motions result in altered capacities of the kinetic chain, and they are modifiable, then interventions to optimize them are essential for counteracting their negative effects (lower back pain, groin/adductor strains, labral tears, etc.).
Assessing your athletes’ hip internal rotation capacity is a great place to start before applying any intervention.
When assessing HIR it is important to differentiate between the potential drivers of loss of motion:
IR at 90 degrees of hip flexion in supine= Primary restriction Glute Max (below image on left is HIR)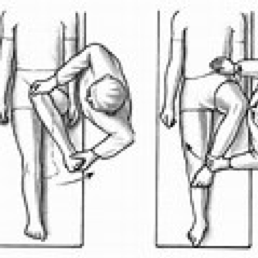
IR at 0 degrees of hip flexion in supine (below image on left is HIR)
On the above assessment you’re just looking for ease of motion and whether or not you can get the femur to rotate medially without the pelvis coming along for the ride (dissociation).
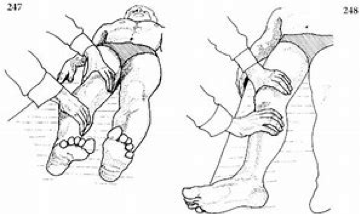
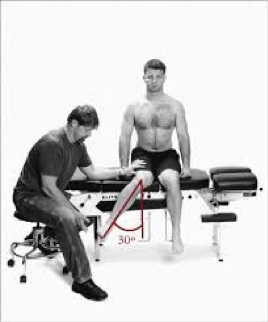
IR at 90 degrees in seated= (most ligamentous structures loosen) primary restriction inferior capsule (glute max/quadratus femoris/obturator)
IR at 0 degrees in prone= (posterior capsule/osseous changes) generally takes muscles out of equation with the exception of small ERs (quadratus femoris/obturator)
If HIR gets better in prone it’s likely a muscular restriction. If it doesn’t it’s more likely to be related to capsular restriction (modifiable) or bony restriction (non-modifiable).
In the above assessments “normative” range is considered 40 degrees* of HIR. From a performance coach perspective rather than any specific number, I’m more interested in side to side asymmetries, the ease of the motion (is it smooth, does it have a hard end feel, or is the range extremely limited), and do the assessment motions illicit any type of pain or discomfort such as “pinching.” In the case of pain, a pinching sensation, or hard end feel/extremely limited range it would be wise to consult with a skilled physical therapist.
All of the previous assessments are open chain (distal limb is free to move).
It’s also important to assess closed chain hip internal rotation when the lower limb is in contact with the ground. While the open chain tests do provide good information, we want a more complete picture and we get that when the feet are in contact with the ground as they often are in sport.
Lower Quarter Rotation Test
I once heard Physical Therapist Charlie Weingroff state the following:
“Overhead Deep Squat w/ knees over toes (feet straight and shoulder width apart) indicates adequate hip internal rotation for many activities. In rotary sports, I might suggest that if it can be controlled, you probably can’t have enough healthy hip internal rotation.
This is not to suggest that you “train” the squat with this set-up… It does suggest however for the purposes of making your screens/assessments consistent and to evaluate qualities like HIR, it is important to screen with the feet straight ahead and shoulder width apart.
I also use a motor control assessment:
IC Adductor/Glute Med Motor Control Test
If the athlete has HIR ability they will feel both the inner thigh near the groin and the outer hip of the bottom leg. Watch for log rolling or pressing down with the top leg to create leverage. Can they engage the inner thigh and the outer hip (on the bottom leg) at the same time? Yes or no?
This is important because in the stance phase of gait (and when they are optimally positioned to do so) the left inner thigh pulls the femoral head into to the hip capsule while the left glute medius locks the pelvis against the femur.
Once you’ve gone through this battery of assessments and evaluated the needs of your athlete it’s time to get to work and provide an exercise prescription to improve hip internal rotation.
Exercise Selection Hierarchy
Repositioning Techniques
Postural control is low-hanging fruit and this should be addressed first. Ross et al., stated that excessive anterior pelvic tilt reduces hip flexion, adduction, and hip internal rotation. Engaging hamstrings and the internal obliques (IO) and transverse abdominus (TA) to posteriorly orient the pelvis to a more “neutral” alignment may be all that’s required to regain adequate HIR.
Supine 90/90 hip lift
(If pelvic tilt is posterior as opposed to anterior, these drills to correct posterior pelvic tilt may benefit athletes.)
After addressing the sagittal orientation of the pelvis with hamstring activation/IO and TA engagement to posteriorly rotate the pelvis to a more “neutral” position, then we move on to adductor recruitment. Specifically, we need to engage the ischiocondylar (IC) fibers of the posterior head of adductor magnus. These fibers have an internal rotation function. While these fibers have several functions, the one that I will highlight is its ability to pull and seat the femoral head into the hip socket (acetabulum).
Side-lying Adductor pull back
When performing the adductor pull back you should feel your top leg inner thigh engage. If not…
Standing posterior capsule
Next, we move on to address the glute medius on the affected side (limited HIR). In a repositioned pelvis courtesy of the 2 previous exercise strategies (hamstrings/IO/TA and IC Adductor Magnus) the glute medius rolls the femoral acetabular (FA) joint into the acetabulum and secures it there.
Side-lying Supported Glute Med
Once the athlete has demonstrated the ability to execute the previous three repositioning techniques and they “feel” it where they should and you reassess and they now have adequate hip internal rotation capacity and motor control, then you can reinforce this movement quality with more dynamic activities.
Integrated techniques
Lateral Bear Crawl
Rotational press with reach
Lateral step with knee drive and med ball chop
Implement the repositioning exercise strategies into the warm-up/cool down or add them as “active recovery” during training sessions.
Example: 1A Inverted Row, 2A Landmine SLDL, 3A Side lying adductor pull back
I use the integrated techniques as a “bridge” from ground based to the dynamic warm-up. They also work well as part of a circuit/station approach when working with large groups.
Also, prescribe repositioning techniques as homework but keep it simple and only if it’s required. That said, there are no downsides to performing these exercise techniques. They will only serve to maintain and upgrade a movement quality that is often deficient in athletes and is absolutely essential for high performance.
When programming exercises to strengthen the hip or to improve hip mobility, a musculature chain of importance is the flexor chain, particularly the psoas muscle. In addition to improved hip internal rotation, psoas strengthening can also affect athletic performance and overall speed.
Related: Drills To Correct Posterior Pelvic Tilt
Reference:
* The physiology of the joints. Lower limb: Churchill Livingstone; 1970. P.256
 About the Author
About the Author
Coach Phil Loomis is a fitness professional and nutrition coach at Life Time Athletic in Bloomfield, MI as well as a strength and conditioning coach for the Michigan Red Sox in Birmingham, MI. He was also the head coach and CEO of Forever Fit in Troy, MI. He is currently certified as a Strength and Conditioning Specialist, Youth Athletic Development Specialist, Speed and Agility Specialist, Corrective Exercise Specialist, and a Precision Nutrition Certified Coach among others.
Coach Loomis played Division 1 college baseball and it was then that he developed the appreciation for the impact that off-field performance training and nutrition can have for developing athletes. His passion for youth and sports performance lead him to start Forever Fit. His training experience has lead him to develop a deep appreciation for corrective exercise and long-term athletic development strategies. He specializes in functional anatomy and bio-mechanics as they relate to program design and corrective exercise; youth athletic development; and rotational/overhead athlete performance enhancement.
Recommended Athletes Acceleration Products
 | |
| Complete Sports Training |





0 Comments for “Essential Movement Qualities: Hip Internal Rotation”